Search
- Page Path
- HOME > Search
Image of Interest
- Adrenal Gland
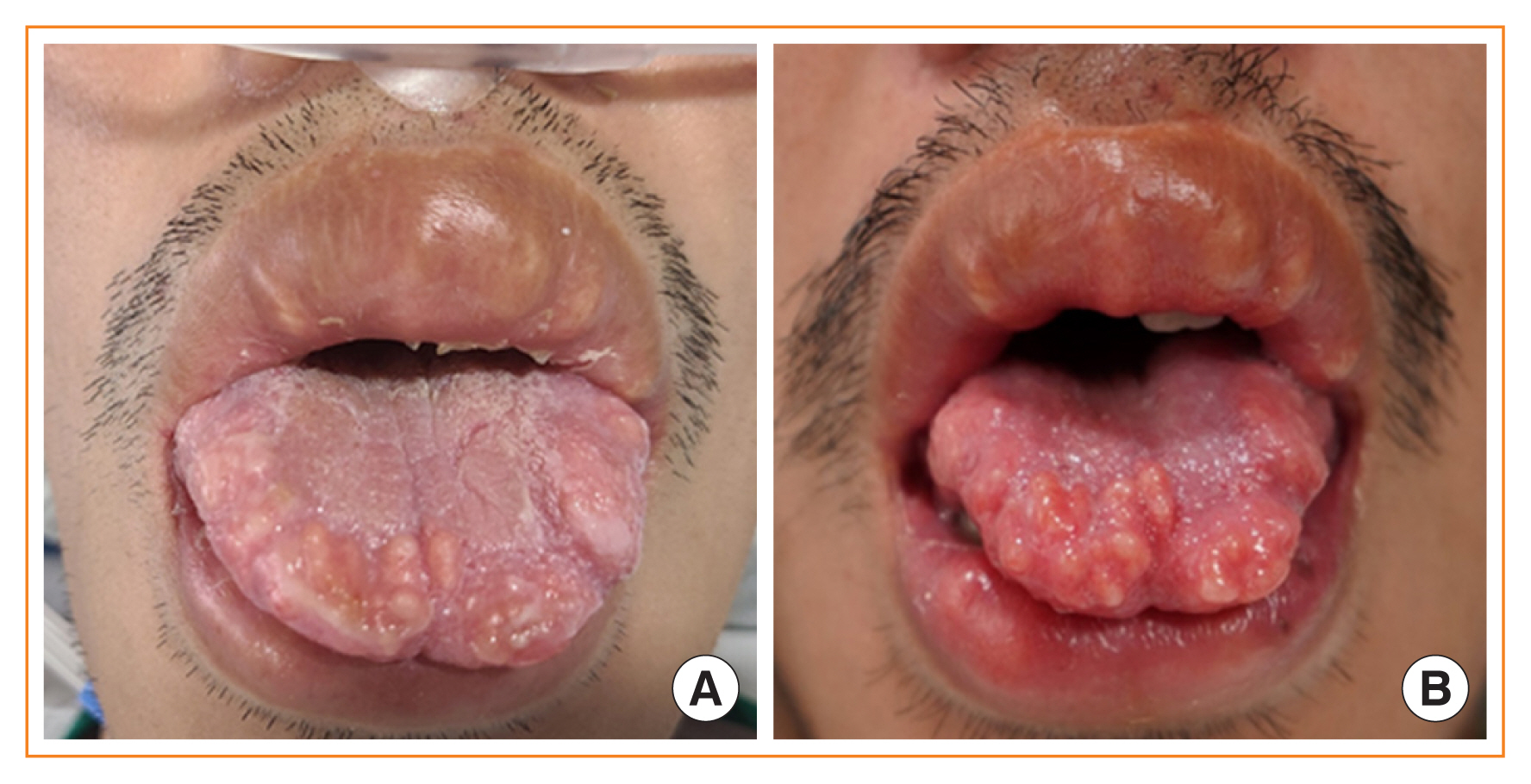
- Mucosal Neuroma Cues for Endocrine Emergency Treatment
- Gyu Gang Choi, Hwan Jin Lee, Hyo Jin Han, Young Beom Jeong, Heung Bum Lee, Ji Hyun Park
- Endocrinol Metab. 2021;36(6):1312-1313. Published online December 3, 2021
- DOI: https://doi.org/10.3803/EnM.2021.1269
- 2,575 View
- 93 Download

Case Reports
- A Case of Simultaneous Presentation of Thyroid Crisis and Diabetic Ketoacidosis.
- Kyung Ae Lee, Kyung Taek Park, Hea Min Yu, Heung Yong Jin, Ji Hyun Park, Hong Sun Baek, Tae Sun Park
- Endocrinol Metab. 2012;27(1):63-67. Published online March 1, 2012
- DOI: https://doi.org/10.3803/EnM.2012.27.1.63
- 2,098 View
- 31 Download
- 1 Crossref
-
 Abstract
Abstract
 PDF
PDF - Two important endocrine emergencies, thyroid crisis and diabetic ketoacidosis (DKA), are uncommon when presented together, but pose serious complications. Without appropriate management, they may result in high mortality. Although several cases of simultaneous presentation of thyroid crisis and DKA have been reported, it is a clinically unusual situation and remains a diagnostic and management challenge in clinical practice. We report rare case with simultaneous presentation of thyroid crisis and DKA without previous warning symptoms. A 23-year-old-woman was brought to the emergency department presenting with acute abdominal pain for one day. She was healthy and there was no personal history of diabetes or thyroid disease. Through careful physical examination and laboratory tests, the patient was diagnosed with thyroid crisis combined with DKA. Concomitance of these two endocrine emergencies led to sudden cardiac arrest, but she was successfully resuscitated. This emphasizes the importance of early recognition and prompt management when the two diseases are presented concomitantly.
-
Citations
Citations to this article as recorded by- Health Behaviors and Risk Factors Associated with Chronic Kidney Disease in Korean Patients with Diabetes: The Fourth Korean National Health and Nutritional Examination Survey
Suk Jeong Lee, Chae Weon Chung
Asian Nursing Research.2014; 8(1): 8. CrossRef
- Health Behaviors and Risk Factors Associated with Chronic Kidney Disease in Korean Patients with Diabetes: The Fourth Korean National Health and Nutritional Examination Survey

- A Case of Concurrent Papillary Thyroid Carcinoma in Familial Medullary Thyroid Microcarcinoma with a Germline C634W Mutation.
- Ji Hye Kim, Ji Hyun Park, Tae Sun Park, Hong Sun Baek, Myoung Ja Chung, Ki Hwan Hong
- Endocrinol Metab. 2010;25(4):354-359. Published online December 1, 2010
- DOI: https://doi.org/10.3803/EnM.2010.25.4.354
- 1,714 View
- 34 Download
-
 Abstract
Abstract
 PDF
PDF - The origins of medullary carcinoma (MTC) and papillary carcinoma (PTC) of the thyroid are embryologically different. Tumors showing concurrent medullary and papillary features are rare and they represent less than 1% of all thyroid malignancies. Hereditary MTC is an autosomal dominantly inherited disease which is genetically determined as part of the MEN 2A, MEN 2B, or variants of MEN 2A such as familial MTC. Germline mutations of the RET gene are the underlying cause of the majority of cases of hereditary medullary carcinomas. The pathogenesis of concurrent PTC with familial MTC has rarely been known. Genetic analysis of the RET oncogene has so far provided conflicting results. Here we describe a family whose sibling was affected by both PTC & MTC, and the family carried a germ-line point mutation in the RET extracellular domain that converted cysteine 634 into tryptophan (C634W).

- Primary Pituitary Abscess: An Unusual Case of Diabetes Insipidus.
- Ji Hye Kim, Ji Hyun Park, Tae Sun Park, Hong Sun Baek
- J Korean Endocr Soc. 2006;21(5):408-413. Published online October 1, 2006
- DOI: https://doi.org/10.3803/jkes.2006.21.5.408
- 1,570 View
- 20 Download
-
 Abstract
Abstract
 PDF
PDF - A 58-year-old man was investigated for his complaints of chronic frontal headache. The endocrinologic hormone studies were compatible with diabetes insipidus and suggestive of panhypopituitarism. Sellar MRI showed a cystic sellar lesion with peripheral rim enhancement after contrast injection, and this led to an initial diagnosis of pituitary adenoma with hemorrhagic necrosis. He underwent an operation via the transsphenoidal approach to access the pituitary gland. During the operation, purulent materials were obtained and no tumor or other associated lesions were detected. There was no evidence of current or previous septicemic illness, meningitis, cavernous sinus thrombosis or sinus infection. All the cultures we obtained were negative. He was put on antibiotics and discharged after 4 weeks. Now, 18 months after treatment, he is doing well.

- The Change of Thyroid Hormone by Short-term Antithyroid Drug Treatment for Preoperative Euthyroidism in TSH-secreting Pituitary Adenoma.
- Min Hee Lee, Ji Hyun Park
- J Korean Endocr Soc. 2005;20(3):261-267. Published online June 1, 2005
- DOI: https://doi.org/10.3803/jkes.2005.20.3.261
- 1,656 View
- 18 Download
-
 Abstract
Abstract
 PDF
PDF - Preoperative euthyroidism is needed to minimize the risk of intraoperative and postoperative complications, such as thyroid storm by surgery. Antithyroid drugs or steroid hormones are commonly used in primary hyperthyroidism for euthyroidism. However, there is no definite consensus for the preoperative management of a TSH secreting pituitary adenoma for the restoration of euthyroidism. Antithyroid drugs are not used for long-term the management of a TSH secreting pituitary adenoma, as they may cause rapid growth and greater invasiveness of the tumor due to a feedback mechanism, but they can be used for short-term management before neurosurgery. We experienced one case of a TSH secreting pituitary adenoma, which showed rapid free thyroid hormone increase due to the short term administration of antithyroid drugs for only 10 days. A somatostatin analogue, octreotide at a dose of 0.1mg, twice a day, was then tried. About 4 weeks later, her serum TSH and free T4 had normalized, with a concomitant clinical improvement. She subsequently underwent an uncomplicated trans-sphenoidal resection of the pituitary adenoma. Antithyroid drugs can induce a rapid thyroid hormone increase, but can only be used for a short-term period, so they should be administered with caution or their use reconsidered


 KES
KES

 First
First Prev
Prev



